A Double-Blind Study
The Influence of Permanent Magnetic Field Therapy on Wound Healing in Suction Lipectomy Patients
Plastic & Reconstructive Surgery: Volume 104(7) December 1999 pp 2261-2266
Man, Daniel M.D.; Man, Boris M.D.; Plosker, Harvey M.D.
Boca Raton, Fla. 851 Meadows Rd., Suite 222; Boca Raton, Fla. 33486
From the Aesthetic Plastic Surgery and Laser Center. Received for publication April 8, 1999; revised June 11, 1999.
Article Outline
Figures/Tables
Abstract (top)
The authors present their experience with the healing influence of permanent magnets on postoperative wounds. The responses of 20 patients who underwent suction lipectomy and postoperative negative magnetic field therapy were studied in a double-blind fashion. Magnets in the form of patches (10 patients) or sham magnet patches (10 patients) were placed over the operative region in each of the patients. Pain, edema, and discoloration (ecchymosis) were evaluated at 1, 2, 3, 4, 7, and 14 days postoperatively. Our results show that the treatment group had significant reductions in pain on postoperative days 1 through 7, in edema on days 1 through 4, and in discoloration on days 1 through 3 when compared with the control group. These results demonstrated that commercially available magnets have a positive influence on the postoperative healing process in suction lipectomy patients.
Modalities potentially capable of improving wound healing carry great interest in plastic surgery. Despite the effort devoted to investigating the effects of different physical modalities on wound healing, few significant advances in the use of any of these new modalities have occurred.
The processes involved in cell and tissue repair and regeneration represent one of the most fundamental properties of complex organisms. Any physical or chemical process capable of improving wound healing merits thorough investigation. In comparison with the advancement and acceptance of magnetic instruments in many other scientific fields, the use of magnetic field energy in the practice of medicine remains extremely limited, despite the fact that magnets for medical treatment are readily available commercially. Both static and time-varying magnetic fields have been successfully applied to treat a variety of musculoskeletal problems. For example, after its description over 25 years ago, the use of electromagnetic fields to help trigger the healing of fracture nonunions1-3 has become an accepted clinical practice worldwide.
Currently, a great deal of activity and interest in studying the effects of magnetic fields on biological organisms exists. On the one hand, grave concerns have been voiced about the potential negative health effects of electromagnetic fields.4,5 On the other hand, many claims are made regarding the use of permanent magnets to treat various types of painful conditions.5-8
Although well-controlled studies have been performed on the stimulation of bone growth by electrical and magnetic fields, the effects of magnetic fields on soft tissues remain unclear; they represent the next frontier in electromagnetic biology and medicine. It has been demonstrated in animal experimental wound models that these modalities can promote healing and increase wound tensile strength.9-12 Electrical and magnetic fields have been associated with a number of demonstrable effects advantageous to wound healing, including increased collagen deposition, enhanced fibroblast migration, increased migration of macrophages and leukocytes leading to decreased bacterial counts, decreased sympathetic vasoconstriction, increased cellular oxygen delivery, and increased wound epithelialization.9-12
Evidence exists that magnetic field therapy can be effective in improving some of the most important factors in wound management, namely, the optimization of the supply of nutrients and oxygen to the treated area. This is of major importance in the case of surgical skin flaps. It is well known that skin flaps exhibit progressive ischemia, with potential tissue necrosis, toward their distal end. An accumulation of neurotransmitters follows the transection of sympathetic nerves during flap elevation, with the resultant vasoconstriction inducing a temporary capillary occlusion within the flap. This sequence of events further involves ischemia followed by reperfusion in the transition zone between adequately perfused proximal tissue and inadequately perfused distal areas. It has been shown in animal studies that the treatment of skin flaps with electric current or magnetic fields may prevent severe ischemia, thus avoiding ischemia/reperfusion injury. However, there are no reports on the use of magnetic fields for the treatment of postsurgical skin flaps in humans.
Any factor that is capable of improving the healing process, especially in the absence of significant side effects, would be of particular interest in plastic surgery. Herein, we present our experience with such a technique: the use of permanent magnetic field therapy in plastic surgical patients.
Patients and Methods (top)
The protocol for this double-blind, randomized study was approved by the Essex Institutional Review Board, Inc. Written informed consent was obtained from 20 patients scheduled to undergo suction lipectomy of various body regions. Patients were randomly assigned to either the treatment group or the control group.
Patient Selection (top)
Enrollment was limited to patients of either sex between the ages of 18 and 75 who were scheduled to undergo suction lipectomy and who had major medical problems. Exclusion criteria included the following:
- Patients unable to give informed consent
- Patients with electronic cardiac pacemakers
- Patients with open wounds
- Patients with infection
- Major medical problems
- Patients with metallic implants at the treatment site
- Skeletal immaturity
Surgical Procedure (top)
The same surgeon performed all suction lipectomies. The areas suctioned included the abdomen, saddlebags, love handles, and thighs, with a variety of areas being suctioned in different patients. A tumescent technique was used in all cases; a 2:1 ratio of tumescent solution was used to aspirate. Ultrasound-assisted suction lipectomy was performed in all patients, and internal ultrasound was employed.
Study Design (top)
The treatment group received magnetic field treatment postoperatively with magnetic devices in the form of patches (Tectonic, Magnetherapy, Inc., North Palm Beach, Florida), which varied in size from 5 ? 15 to 20 ? 30 cm, and in shape (including both square and rectangular). The patches contained ceramic magnets oriented unidirectionally within them, with a total magnetic field strength of from 150 to 400 gauss, depending on the size of the magnetic patch used. The control group had sham patches placed. These sham patches were identical to the magnetic patches in all respects, including having the same ceramic material inside, but they possessed no magnetic activity. All patches were fixed with compressive dressings, with the negative pole of the magnet placed against the skin. The patches were placed on the skin overlying the areas that had been suctioned, with various sizes and shapes of magnets used so as to best fit the area being treated. The patches were applied immediately postoperatively, and they were left in place for a total of 14 days, with the treated areas inspected on postoperative days 1, 2, 3, 4, 7, and 14.
All postoperative assessments were made by the same blinded observer. The patients, surgeon, and observer were all blinded as to which patients had the real or sham magnetic devices.
Discolorations (ecchymoses) within the limits of the area covered by the magnetic patches and the area outside were compared and documented by the same observer on a scale of 0 to 10, with 0 representing a completely normal skin color, with no discoloration at all, and 10 representing severe ecchymosis covering the entire area, with a dark blue/violet color and no normal skin color showing through. Edema was also assessed by the same blinded observer on a scale of 0 to 10, with 0 representing no edema when compared with neighboring regions that had not undergone any surgery, and 10 representing marked swelling, with a shiny skin surface due to stretching of the overlying skin.
Pain was assessed by means of a visual analog pain scale throughout the study period. While in the facility, this was recorded by our blinded observer. Once the patients were discharged, this was accomplished by having the patients keep a log of their pain scores on a daily basis.
Statistical Analysis (top)
All data were subjected to statistical analysis, and the results are presented as means and standard deviations. On the basis of the nature of the data and its distribution, nonparametric statistical tests were used in analyzing the data. Discoloration, edema, and pain scores were compared between groups at each time interval using the Wilcoxon rank sum test and the Kruskal-Wallis test. p < 0.05 was considered statistically significant.
Results (top)
Patient demographics were similar between the two study groups with regard to age, sex, volume of tumescent solution used, and volume aspirated.
In the treatment group, a statistically significant decrease (p < 0.05) in discoloration occurred when compared with the control group on postoperative days 1, 2, and 3. The magnitude of the reduction in discoloration was also clinically significant, ranging from 43 percent on postoperative day 1 to 28 percent on postoperative day 3. By postoperative days 4, 7, and 14, there was no longer any significant difference in discoloration between the two groups (Fig. 1; Table I).
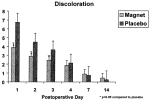 Fig. 1. Postoperative discoloration after suction lipectomy in patients treated with magnet patches versus placebo patches. Values are means and standard deviations.
Fig. 1. Postoperative discoloration after suction lipectomy in patients treated with magnet patches versus placebo patches. Values are means and standard deviations.
![]() Table I. Postoperative Edema, Discoloration, and Pain after Suction Lipectomy in Patients Treated with Magnet Patches or Placebo Patches
Table I. Postoperative Edema, Discoloration, and Pain after Suction Lipectomy in Patients Treated with Magnet Patches or Placebo Patches
With regard to edema, a statistically significant decrease (p &.05) in edema occurred in the treatment group when compared with the control group on postoperative days 1, 2, 3, and 4. The reductions in edema on days 1 through 4 were clinically significant as well, varying from 40 to 53 percent when compared with the control group. By postoperative days 7 and 14, although there continued to be some decrease in edema, it was no longer statistically significant (Fig. 2; Table I).
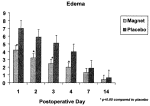 Fig. 2. Postoperative edema after suction lipectomy in patients treated with magnet patches versus placebo patches. Values are means and standard deviations.
Fig. 2. Postoperative edema after suction lipectomy in patients treated with magnet patches versus placebo patches. Values are means and standard deviations.
When compared with the control group, pain was significantly decreased (p < 0.05) in the treatment group on postoperative days 1, 2, 3, 4, and 7. By postoperative day 14, although the pain scores continued to be lower in the treatment group, the difference was not statistically significant (Fig. 3; Table I). The patients in the treatment group felt noticeably better, demonstrating a 37 to 65 percent decrease in pain when compared with the control group, leading to a decreased consumption of analgesic medications.
 Fig. 3. Postoperative pain (as measured by visual analog scale scores) after suction lipectomy in patients treated with magnet patches versus placebo patches. Values are means and standard deviations.
Fig. 3. Postoperative pain (as measured by visual analog scale scores) after suction lipectomy in patients treated with magnet patches versus placebo patches. Values are means and standard deviations.
There was no difference in the incidence of adverse events between the treatment group and the control group throughout the study period. No side effects were observed in either group.
Figures 4 through 6 illustrate patients after suction lipectomy and demonstrate the virtually complete disappearance of ecchymoses 48 hours after the application of the magnet patch, except beyond the border of the magnet patch where discoloration was still visible.
 Fig. 4. (Left) Abdomen 48 hours after suction lipectomy, with magnet patch in place. Note ecchymosis and discoloration of the abdomen. (Right) Abdomen 48 hours after surgery and the application of the magnet patch, with discoloration markedly diminished in the area covered by the magnetic patch.
Fig. 4. (Left) Abdomen 48 hours after suction lipectomy, with magnet patch in place. Note ecchymosis and discoloration of the abdomen. (Right) Abdomen 48 hours after surgery and the application of the magnet patch, with discoloration markedly diminished in the area covered by the magnetic patch.
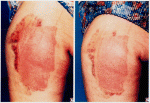 Fig. 5. (Left) Ecchymosis and discoloration 24 hours after suction lipectomy and treatment with the magnetic patch. (Right) Operative site 72 hours postoperatively. Note the virtually complete disappearance of discoloration, other than that beyond the borders of the magnetic patch, at both intervals.
Fig. 5. (Left) Ecchymosis and discoloration 24 hours after suction lipectomy and treatment with the magnetic patch. (Right) Operative site 72 hours postoperatively. Note the virtually complete disappearance of discoloration, other than that beyond the borders of the magnetic patch, at both intervals.
 Fig. 6. (Left) Thigh 72 hours after suction lipectomy, with magnet patch in place. Note the marked ecchymosis and discoloration. (Right) Thigh 72 hours after suction lipectomy with magnet patch removed, showing markedly diminished ecchymosis and discoloration within the area covered by the magnetic patch.
Fig. 6. (Left) Thigh 72 hours after suction lipectomy, with magnet patch in place. Note the marked ecchymosis and discoloration. (Right) Thigh 72 hours after suction lipectomy with magnet patch removed, showing markedly diminished ecchymosis and discoloration within the area covered by the magnetic patch.
Discussion (top)
Much of the theoretical basis for the postoperative use of magnetic stimulation is based on the work of Becker,5 who theorized the existence of an electromagnetic system in the body that controlled tissue healing. When the electrical balance of the body is disturbed by an injury, an injury current is generated, with the resulting shift in the body’s current triggering a set of biological repair systems. As healing progresses, this current of injury decreases until it reaches zero, at which time the healing process is complete.8 This is the basis of the manner in which externally applied magnetic fields are thought to stimulate biological homeostatic feedback mechanisms and trigger the events that result in tissue repair.
The healing process is accompanied by many dynamic processes and events, the most obvious and troublesome of which include pain, swelling, erythema, and diminished function. The beneficial effects of magnetic fields that may be of particular benefit to surgical patients include a reduction of edema, an increase in cellular oxygen delivery, an anti-inflammatory effect, and an analgesic effect.9-12 One possible mechanism by which magnetic fields may exert these effects is by enhancing blood flow to the site of injury, thereby increasing oxygen delivery and speeding the overall healing process.13,14
In our group of study patients, magnetic field therapy was quite remarkable in both the prevention and treatment of these signs and symptoms and also in the alleviation of pain itself. The magnitude of the reduction in postoperative pain was quite significant, allowing for a decrease in the need for analgesic medication. In procedures in which significant ecchymoses or hematomas occur, one would normally expect manifestations such as these to take at least 2 to 3 weeks to resolve, whereas with the use of magnetic field therapy, they resolved in 48 to 72 hours, as is well demonstrated by the photographs (Figs. 4 through 6).
Although the application of any padding has the potential to reduce edema and ecchymosis, we think that our control group, who used identical, nonmagnetized pads, demonstrated that this factor alone did not account for the improvement. This is evidenced by the significantly greater reduction in edema and ecchymosis found in the treatment group.
Conclusions (top)
In this first attempt to use postoperative magnetic field therapy in plastic surgical patients, a beneficial effect was clearly exerted; it markedly ameliorated many of the undesirable factors associated with the healing process, with no side effects observed. In view of this apparent efficacy and the freedom from adverse effects, this modality certainly appears promising, and it merits further investigation.
Daniel Man, M.D.
851 Meadows Rd., Suite 222; Boca Raton, Fla. 33486; info@drman.com
Acknowledgment (top)
We thank Edsel Baker, M.S., of the Statistics Department at the University of Florida for the statistical analysis.
REFERENCES (top)
- Friedenberg, Z. B., Harlow, M. C., and Brighton, C. T. Healing of nonunion of the medical malleolus by means of direct current: A case report. J. Trauma 11: 883, 1971.
- Bassett, A. C. Fundamental and practical aspects of therapeutic uses of pulsed electromagnetic fields (PEMFs). Crit. Rev. Biomed. Eng. 17: 451, 1989.
- Sharrard, W. J. W. A double-blind trial of pulsed electromagnetic fields for delayed union of tibial fractures. J. Bone Joint Surg. Br. 72: 347, 1990.
- Wilson, R. Risk assessment of EMF on health. IEEE Eng. Med. Biol. 15: 77, 1996.
- Becker, R. O. Cross Currents, The Perils of Electropollution, The Promise of Electromedicine. New York: G. P. Putnam’s Sons, 1990.
- Altman, L. K. Study on using magnets to treat pain surprises skeptics. New York Times, December 9, 1997.
- Horstman, J. Explorations: Magnets. Arthritis Today 12: 48, 1998.
- Vallbona, C., Hazelwood, C. F., and Jurida, G. Response of pain to static magnetic fields in postpolio patients: A double-blind pilot study. Arch. Phys. Med. Rehabil. 78: 1200, 1997.
- Foulds, I. S., and Barker, A. T. Human skin battery potentials and their role in wound healing. Br. J. Dermatol. 109: 515, 1983.
- Jaffe, L. F., and Vanable, J. W., Jr. Electric fields and wound healing. Clin. Dermatol. 2: 34, 1984.
- Weiss, D. S., Kirsner, R., and Eaglstein, W. H. Electrical stimulation and wound healing. Arch. Dermatol. 126: 222, 1990.
- Markov, M. S. Electric current and electromagnetic field effects on soft tissue: Implication for wound healing. Wounds 7: 94, 1995.
- Lednev, V. V. Possible mechanisms for the influence of weak magnetic fields on biological systems. Bioelectromagnetics 12: 71, 1991.
- Mayrovitz, H., and Larsen, P. B. Effects of pulsed electromagnetic fields on skin microvascular blood perfusion. Wounds 4: 197, 1992.
1999 American Society of Plastic Surgeons
